
Andrew M. Ibrahim MD, MSc, FACS
General Surgeon at University of Michigan, Chief Clinical Officer at Viz.ai
Rural communities face persistent gaps in healthcare access, quality, and outcomes that leave patients underserved and health indicators worse than in urban areas. Now, AI can directly address these rural care barriers.

More than 4.4 million Ohio residents live in rural communities across 73 counties with a significant rural footprint. To improve access to care statewide, the Ohio Rural Health Transformation Program plans to establish Rural Health Innovation Hubs that connect clinically integrated networks, regional centers of excellence, and pharmacy networks across the continuum of care.
This is a complex challenge. Ohio’s rural communities are geographically dispersed and often sparsely populated, making timely access to care difficult. In many areas, patients must travel long distances to reach hospitals or specialty services, and some counties lack local healthcare facilities altogether.
Access to care is further strained by workforce shortages and a high burden of chronic disease. Rural areas have significantly fewer providers than the state average, and rural populations tend to be older, with higher rates of heart disease, diabetes, obesity, and stroke. Heart disease mortality remains higher in rural communities than across Ohio overall, highlighting the urgency of earlier identification and better care coordination.
Viz.ai’s platform provides AI-powered disease detection and intelligent care coordination, helping rural providers manage complex and time-sensitive conditions more effectively, without adding workflow burden.
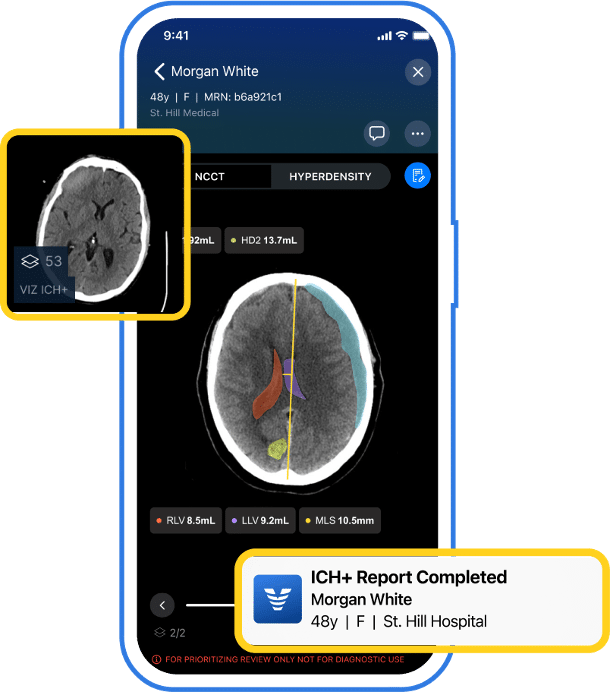
Specialists can review 3D imaging alongside an AI-generated patient summary built from ambient listening and EHR data, and make referrals directly within Viz.ai’s HIPAA-compliant mobile app. This accelerates diagnosis and streamlines coordination across care teams.
Viz.ai helps rural Ohio health systems:
Together, these capabilities help deliver faster care, better access, and more sustainable rural healthcare across Ohio.
1
Early detection and triage at the point of care
AI can rapidly analyze imaging and clinical data to flag suspected disease and critical findings in minutes, even in hospitals without on-site specialty coverage. This accelerates diagnosis and enables faster treatment or transfer decisions.
2
Decision support for rural care teams
Rural emergency departments are often staffed by generalists managing high-acuity cases. AI tools support guideline-based decision-making by surfacing and sharing actionable insights in real time, mitigating workforce shortages without replacing clinical judgment.
3
Care coordination across fragmented systems
Critical and acute care frequently require coordination across EMS, emergency departments, imaging, specialists, and receiving centers. AI platforms like Viz.ai unify these workflows, ensuring the right teams are alerted and aligned quickly—critical in rural settings.
AI software for stroke is recognized in American Heart Association (AHA) guidelines as a tool to support early detection, triage, and clinical decision-making in acute stroke care.
This matters for rural health policy. The inclusion of AI in AHA guidelines signals that these technologies are clinically validated, evidence-based, and appropriate for broad adoption, not pilot-only experimentation.
In rural settings, platforms like Viz.ai can enable faster identification of suspected disease, support earlier activation of care and transfer pathways, reduce time to treatment, and improve consistency of care across low-volume and resource-constrained hospitals.
Hear from Dr. Andrew Ibrahim, Chief Clinical Officer at Viz.ai, in a congressional hearing on AI in healthcare, on how AI-powered care coordination specifically helps rural communities and patients.