
Andrew M. Ibrahim MD, MSc, FACS
General Surgeon at University of Michigan, Chief Clinical Officer at Viz.ai
Rural communities face persistent gaps in healthcare access, quality, and outcomes that leave patients underserved and health indicators worse than in urban areas. Now, AI can directly address these rural care barriers.

Rural hospitals face structural challenges that make timely care more difficult to deliver, including limited specialty coverage, fragmented care coordination, and constrained operational resources.
AI-powered care coordination platforms can help address these challenges by enabling rural health systems to demonstrate measurable progress in the areas that matter most for state rural health transformation programs: clinical outcomes, specialty access, and healthcare utilization.
1
Faster treatment and improved clinical outcomes
AI can rapidly analyze imaging and clinical data to identify high-risk patients and activate the appropriate care teams for time-sensitive conditions such as stroke, myocardial infarction, and pulmonary embolism. By accelerating diagnosis and treatment decisions, rural providers can reduce delays, improve clinical performance metrics, and deliver better patient outcomes when minutes matter most.
2
Expanded specialty access for rural care teams
Rural emergency departments are often staffed by generalists managing complex and high-acuity cases without immediate access to specialty expertise. AI-powered care coordination platforms connect frontline clinicians with remote specialists in real time, enabling faster consultation, more coordinated decision-making, and stronger collaboration across care teams.
3
Reduced healthcare utilization and avoidable transfers
Critical and acute care often requires coordination across EMS, emergency departments, imaging teams, specialists, and referral centers. AI-powered platforms unify these workflows, helping clinicians determine the most appropriate care pathway and align the right teams quickly. This improves system efficiency, reduces unnecessary transfers, and helps rural hospitals preserve capacity while delivering better patient experiences.
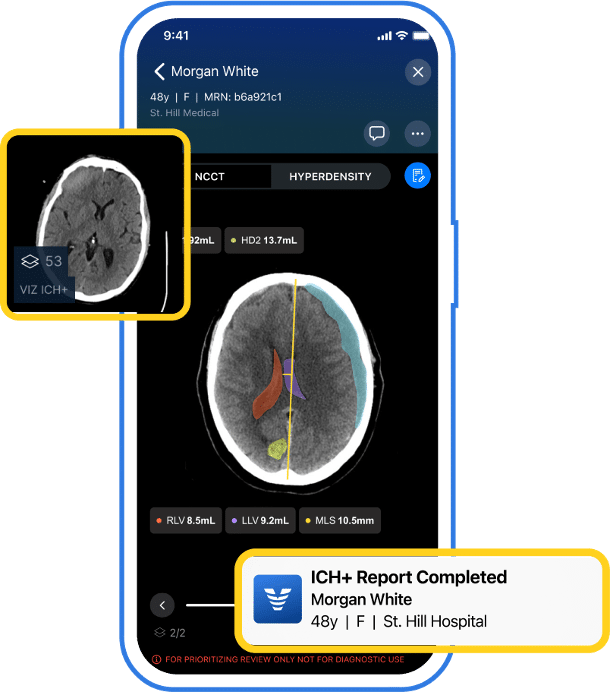
Stroke care illustrates how AI-powered care coordination can transform time-sensitive care in rural environments.
Stroke is a leading cause of death and long-term disability, with rural patients experiencing higher mortality and longer treatment delays. These gaps are driven by structural barriers, such as limited access to neurologists, imaging expertise, and coordinated stroke systems—not lack of clinical effort.
Because stroke is profoundly time-sensitive, delays disproportionately harm rural patients, making it a clear opportunity for meaningful rural health transformation.
AI platforms can help rural hospitals identify suspected stroke earlier, notify specialists faster, and coordinate transfers when needed—helping patients receive appropriate care more quickly.
AI software for stroke is recognized in American Heart Association (AHA) guidelines as a tool to support early detection, triage, and clinical decision-making in acute stroke care. 
This matters for rural health policy. The inclusion of AI in AHA guidelines signals that these technologies are clinically validated, evidence-based, and appropriate for broad adoption—not pilot-only experimentation.
In rural settings, platforms like Viz.ai can enable:
Beyond stroke, the same platform infrastructure can support additional service lines—including cardiology, trauma, oncology, and pulmonary care—allowing rural health systems to scale impact across multiple clinical pathways.
In rural settings, platforms like Viz.ai can enable faster identification of suspected disease, support earlier activation of care and transfer pathways, reduce time to treatment, and improve consistency of care across low-volume and resource-constrained hospitals.
Hear from Dr. Andrew Ibrahim, Chief Clinical Officer at Viz.ai, in a congressional hearing on AI in healthcare, on how AI-powered care coordination specifically helps rural communities and patients.